Introduction
Earlier this year, I decided to leave my job and take a break to explore my next career move. Despite the challenging economic situation, I feel incredibly fortunate to have found something truly exciting. (If you're in the field of product management or data science/engineering and looking for a job, please don't hesitate to reach out!)
During the initial phase of my hiatus, I encountered something completely new to me: the realization that starting the next day, I would be without health insurance. While still employed, I had heard about COBRA, but it hadn't occupied much of my thoughts. When I looked up the details of the COBRA plan, I was shocked to find that it would be ten times more expensive than the coverage I had through my employer. I began researching self-insured plans that some of my previous employers had used. This led me to United's short-term insurance plans, where I found myself navigating through a daunting list of 160 different options. After numerous calls with brokers over three days, I finally managed to secure a plan that I could barely afford, providing me with only basic coverage. Even then, it excluded specialist visits and required high co-pays even for seeing my primary doctor. Needless to say, navigating the complexities of health insurance in America is a challenging task, particularly for individuals like myself.
However, amidst the difficulties, there is a silver lining. The healthcare payer space is currently undergoing significant innovation. I find the energy and the wide array of emerging solutions in the past decade, particularly the last five years, truly inspiring. Yet, with this rapid evolution, there are also gaps in understanding and a complex landscape that requires careful examination. As I write this, I am on a learning journey myself, and I hope that we can navigate this terrain together.
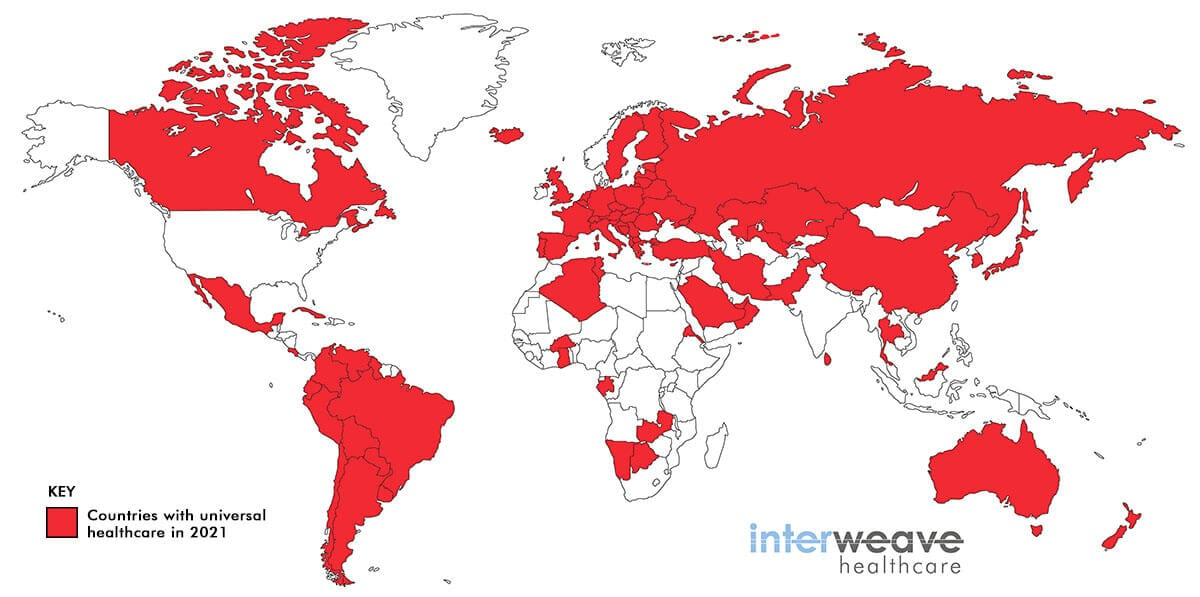
The US stands alone among the strong economies (even India has a very well-established network of government hospitals albeit the quality of care struggles compared to private hospitals). How did we get here?
Let’s start with a brief history.
History of Health Insurance in the US
Before 1900:
Healthcare payments were mostly out of pocket. Fees by physicians and hospitals were directly charged to patients.
Early 1900s:
In the early 1900s, the emergence of employer-sponsored health insurance began. Some employers started offering health benefits to attract and retain workers. There was relatively strong opposition, even in the beginning, to government-funded plans or any government involvement in health insurance.
1920s-1940s:
During the Great Depression, healthcare costs became a burden for many individuals. This led to the rise of prepaid group practice, where individuals paid a fixed fee to access healthcare services provided by a specific group of physicians.
In 1939, the Baylor University Hospital in Texas implemented a prepayment plan, which is considered the first true health insurance plan. It covered a group of schoolteachers and became the basis for Blue Cross plans.
Mid-20th Century:
World War II (1939-1945) brought wage freezes, and employers began offering health insurance benefits as a way to attract workers without violating wage controls.
In 1943, the Internal Revenue Service (IRS) ruled that employer contributions to health insurance would be tax-exempt, leading to the widespread adoption of employer-sponsored health coverage.
Blue Cross and Blue Shield plans expanded across the country, providing coverage for hospital and medical services, respectively.
1960s-1970s:
In 1965, the Medicare and Medicaid programs were established as part of the Social Security Amendments. Medicare provided health insurance for individuals aged 65 and older, while Medicaid offered coverage for low-income individuals and families.
The rise of managed care organizations (MCOs) began in the 1970s. MCOs aimed to control costs by coordinating care and implementing utilization management techniques.
1980s-1990s:
Health Maintenance Organizations (HMOs) gained popularity as a form of managed care. They emphasized preventive care, required patients to select a primary care physician, and often limited coverage to a specific network of providers.
Preferred Provider Organizations (PPOs) also emerged, offering more flexibility in choosing healthcare providers.
The Consolidated Omnibus Budget Reconciliation Act (COBRA) of 1985 allowed workers to continue their employer-sponsored health coverage for a limited period after leaving a job.
21st Century:
The Affordable Care Act (ACA), signed into law in 2010, introduced significant changes to the healthcare system. It aimed to expand access to insurance coverage, establish health insurance marketplaces, and implement insurance reforms such as prohibiting denial of coverage based on pre-existing conditions.
The ACA also created health insurance subsidies and penalties for individuals who did not obtain insurance.
Medicaid expansion was a key provision of the ACA, although its implementation varied across states due to a Supreme Court ruling in 2012.
Various reforms and adjustments have been proposed and implemented since the ACA, reflecting ongoing debates and efforts to improve the U.S. healthcare system.
The Different Base Payer Models in the US
While there are payers, and intermediaries spinning up in many forms, the offerings can largely be categorized as follows:
Fee-for-Service (FFS):
This is a traditional payment model where healthcare providers are reimbursed for each service or procedure they perform. The payment is typically based on a predetermined fee schedule or a negotiated rate between the provider and the payer. FFS can incentivize volume-based care and may not necessarily prioritize quality or outcomes.
Capitation:
In this model, healthcare providers are paid a fixed amount per patient or enrollee, usually every month. The payment is irrespective of the actual services provided or the number of visits. The provider assumes the financial risk of providing necessary care within the allocated amount. Capitation can encourage preventive care and cost-effective management but may also result in the underutilization of services.
Bundled Payments:
This model involves making a single payment for a defined episode of care or a specific set of services related to a particular condition or procedure. The payment covers all the necessary services provided by multiple providers involved in the patient's care during that episode. Bundled payments aim to promote coordination among providers and reduce fragmented care.
Pay-for-Performance:
Also known as value-based reimbursement, this model ties payment to the quality and outcomes of care. Providers receive financial incentives or penalties based on their performance on specific quality measures or metrics. Pay for performance aims to improve the quality of care, patient outcomes, and cost-effectiveness.
Accountable Care Organizations (ACOs):
ACOs are networks of healthcare providers, including hospitals, physicians, and other healthcare professionals, who collaborate to provide coordinated care to a defined population. ACOs are responsible for the quality and cost of care for their enrolled patients. They may operate under various payment models, such as shared savings or shared risk arrangements.
Government Programs:
These include government-funded healthcare programs like Medicare (for elderly and certain disabled individuals) and Medicaid (for low-income individuals and families). These programs have their own payment models, rules, and regulations for reimbursement to healthcare providers.
Self-Pay:
This model involves individuals paying for healthcare services out of their own pockets, without involvement from insurance companies or third-party payers.
Who offers these plans?
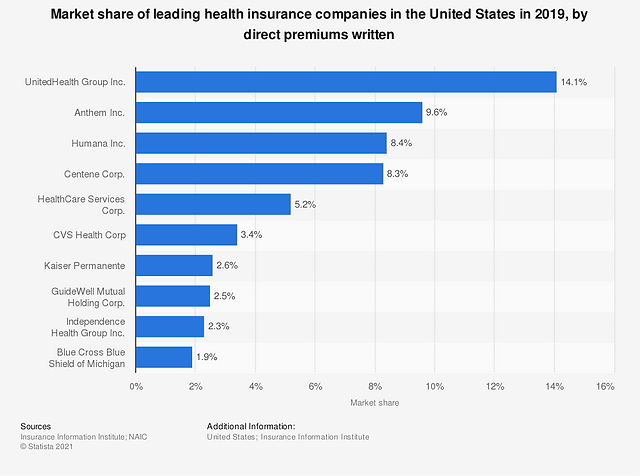
Private Large Health Insurance Companies:
These are the familiar types of insurance companies that we often encounter. Companies like United or Cigna collaborate with employers to provide a range of plan options, such as HMO, PPO, EPO, and more (we will discuss these plans in detail later). These health insurance companies not only partner with employers but also offer various solutions beyond that. As mentioned earlier, they collaborate with or own smaller insurance companies that can provide short-term medical plans and tri-term medical plans for individuals and families.
A significant portion of these companies' business also involves offering Medicare Advantage plans. Medicare Advantage plans operate on annual contracts with Medicare. They provide the same benefits as the Part A and Part B Medicare plans, which are available to individuals aged 65 and above (in some cases even before 65). The insurance companies offering these plans must reapply and renew their contracts each year. Consequently, the plan's benefits, network, and costs may change from one year to another.
Government:
The U.S. government directly offers a wide range of plans, such as Medicare (for individuals aged 65+), Medicaid (for low-income families and individuals), Children's Health Insurance Program (CHIP), Veterans Health Administration (VHA), Indian Health Service (IHS), and Affordable Care Act (ACA) plans.
While most of these programs are overseen by the Centers for Medicare and Medicaid Services (CMS), individual insurance companies partner with CMS to manage, offer, and regulate these plans. CMS plays a role in the administration and oversight of the Health Insurance Marketplace established under the Affordable Care Act (ACA). It manages the eligibility and enrollment process, sets standards for qualified health plans (QHPs) offered on the Marketplace, and provides guidance to states and insurance issuers regarding the Marketplace's operation. In the case of IHS, services are delivered through IHS-operated facilities, tribal health programs, and urban Indian health centers.
Smaller (but exciting and innovative) Health Insurance Companies:
This is where most of the innovation in the health insurance industry is taking place. Smaller companies have emerged to improve the industry by cutting costs and tailoring health insurance plans to individual needs. Traditional health insurance plans are considered outdated and not aligned with the diverse needs individuals face in various aspects of their health. Many of these companies initially focused on point solutions. For instance, Oscar Health, founded in 2012, concentrated on virtual care and reducing drug costs. Omada emerged, partnering closely with individuals, employers, and health plans, with a focus on virtual care for chronic conditions such as musculoskeletal (MSK) issues, obesity, as well as assisting members with behavioral and lifestyle changes.

The tip of iceberg of innovative health insurance solutions that we will dive deeper into in my coming posts Since then, companies have expanded their focus to include employers and helping fellow startups offer health insurance to their employees. While point solutions remain important, self-funding has become a significant component. Companies now assist employers in designing customized plans based on their size and the characteristics of their employee population.
This is just the tip of the iceberg as far as understanding the different health plans and plan providers. I plan to go deeper into each of these plan types including the innovation that tech companies are bringing in my next post.



Great post Rikin - a really nice summary that hasn't been matched anywhere - so much so that I've saved it for future reference.