Options for and Innovation in health insurance
You don't want to miss this one, I learned a lot doing my research and I hope you do too
I hope everyone had a great 4th of July! Mine was great, we had a family bbq and then I spent an hour canceling my short-term health insurance plan after I started coverage from my employer, it wasn’t fun, as I expected! Anyways, let’s geek about why navigating insurance sucks and how some companies are working to make it better.
In my last post, we looked at a brief history of health insurance in America and reviewed the different types of plans that health insurers offer on a high level and who these health insurers are. The reality is that this top layer of health plan types has a lot of complexity underneath and founders in digital health have realized that there is a lot more room for innovation and much more to offer individuals and groups in terms of coverage.
Employer Coverage
Most people in the US are covered by their employers. However, population characteristics are different, not just in terms of health but also access and affordability. For example, think about a small business that is made up of a few hundred employees (which is a lot of startups today), who have a relatively high-risk profile because the average age of the employees is a lot higher than the groups in an average company. Should the employer be forced to pay high premiums or transfer the price to the cost to its employees?
Depending on the size and the willingness to bear risk, some employers can purchase group health plans (similar to average-sized and larger employers everyone is familiar with) or self-fund. For much smaller groups, the employer is not legally obligated to provide health insurance and employees can look at short-term insurance plans, get coverage through their spouse, or look at exchange plans (more on this below). Largely, there are three ways that an employer can offer health insurance:
Fully Insured: Employers pay a monthly premium to the health insurance company that covers the costs of claims and care of all employees. The premiums are standard for the employer and the employee (usually a small cost passed on to the employee). The insurance plan is a win if employees are uncharacteristically unhealthy or end up visiting the doctor a lot/spending a lot of money on their healthcare. It is a waste if employees are generally healthy and do not use much of their benefits.
Self-Funded: Employers pay the employees’ health claims instead of paying a premium and rely on their employees staying healthy overall as a group. If a few employees start to make a lot of claims and spend a lot more on their healthcare, the employer can end up bearing high costs. There is usually a stop loss to cover after a limit (an employer “deductible” in a sense). It is larger businesses that usually stick to this, combining a broker or third party (that manages their claims) with a stop-loss option. This is a costly option in general if you are a smaller employer or have a medium-high likelihood of having an unhealthy population.
Hybrid: These plans combine fully insured plans with self-insured ones. Employers work with a third-party or a large insurance carrier directly. The monthly premiums are set based on risk - predictability (usually calculated with the help of a third party, broker, or carrier). At the end of the insurance term (usually 12 months from open enrollment), the employer is liable for stop-loss, if the group makes claims that amount more than the estimated costs in the risk prediction or is eligible for reimbursement if the costs are lower.
One thing is clear, the point solution providers and third-party partners that manage claims and coordinate insurance are extremely important in this setup. Just think about the various things an employer has to take care of (which they usually do through a broker): finding the right risk profile for their employee pool, negotiating rates, claims administration and payments, setting up drug supplemental coverage, wellness benefits, and customers services for their members. Needless to say, this is where a good number of healthcare founders have dedicated their efforts and where a lot of innovation is happening in the payer space.
Speaking of Third Parties or Third Party Administrators (TPAs) as they are usually called in payer lingo, Collective Health is an all-inclusive TPA that does administration, navigation, and support. Collective partners with top insurance carriers and provides a platform for employers and employees to manage their group/individual costs and benefits. The platform helps create a unique profile for the organization, helps employers mix and match insurance solutions, and pushes members to pursue preventative rather than curative care. Some of the results are impressive: A 50% reduction in costs over a five-year period for Collective’s members and 25% lower utilization than the national average (although the statistics don’t mention if the national average greatly differs from employer populations similar to the ones that Collective partners with).
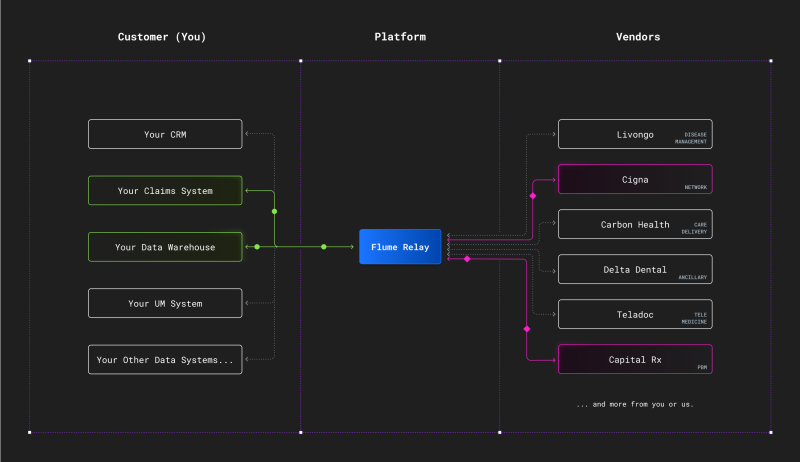
Other, smaller solutions are focusing on one or more TPA tasks. Take Flume Health for example which focuses on the communication layer between payers and vendors (providers delivering directly to the user ex: telemedicine providers or drug benefit managers who work directly with the user). Flume Relay is an automation platform that acts as a universal translation layer for information exchange between payers and vendors. Its simplicity allows anyone to set up and manage data exchanges with different solutions, a practice that is becoming more and more common with employers building customized plans in which they partner with multiple carrier/point solutions.
Self Coverage:
On a high level, there are many options for individuals to obtain health insurance without relying on an employer-sponsored plan:
Health Insurance Marketplace: Enacted in 2010, the Affordable Care Act (ACA) expanded health insurance coverage to more than 20 million people and made coverage more affordable. Individuals can purchase health insurance plans on the government-run Health Insurance Marketplace. These marketplaces offer a range of options from different insurance providers, and individuals may be eligible for subsidies or tax credits based on their income. These marketplace plans have multiple options that are available to people through employers in general such as HMO, PPO, and POS.
Medicare: Medicare provides healthcare to seniors and individuals with certain disabilities. It is funded through a combination of payroll taxes, premiums paid by beneficiaries, and general government revenues. Medicare is usually provided as a fee for service in the form of Part A and Part B (hospital insurance) or Part C as medicare advantage, which is administered by private health insurance companies that are vetted by the CMS. In all cases, individuals must sign up for Part D (drug coverage), which they must sign up for separately if they have Part A and Part B and is usually included with Part C.
Medicaid: Medicaid is a state and federal program that provides health coverage to low-income individuals and families. Eligibility criteria vary by state, but generally, individuals with limited income and resources can qualify for Medicaid.
TriCare and VA: These insurance plans are reserved specifically for the Military and Veterans respectively and administered by the Department of Defense.
Individual Health Insurance Plans: Insurance companies offer individual health insurance plans that individuals can purchase directly. These plans consist of short-term and month-to-month insurance options and are usually available throughout the year and aren’t restricted to open enrollment.
COBRA: COBRA (Consolidated Omnibus Budget Reconciliation Act) allows individuals who have recently left their jobs, and thus lost their employer-sponsored health insurance, to continue their coverage for a limited period. COBRA coverage is usually expensive since the individual is responsible for paying the full premium.
Catastrophic Health Insurance: Catastrophic health insurance plans are designed to provide coverage for severe and costly medical events. These plans have lower premiums but high deductibles and are primarily meant for young and healthy individuals.
We already discussed some of the smaller insurers who focused on certain buckets of the population or offer insurance directly in my last post but here is some more on these companies:
Devoted Health focused on Medicare populations and offered its own option of Medicare Advantage (MA). They differentiated their MA plans from other carriers by partnering with high-quality providers as well as providing extended virtual and in-home care. By identifying gaps in legacy carrier offerings, Devoted was able to offer more to the elderly population and focus on improving benefits that are more relevant.
Most individuals spend most of their care in the primary care setting. Therefore, it has become important for insurance providers to improve primary care access and this is what Taro Health is focusing on. Taro offers unique plans on the market with 0$ primary care and mental health. Taro has already partnered with over 100,000+ providers, 4000 hospitals, and 75000+ pharmacies in the state of Maine. Startups are either focusing on the care side or the payer side when it comes to primary care. Expect to see similar solutions across the U.S. that focus on the middle-aged and middle-class population that is looking for better and cheaper access to these benefits and is in need of point solutions.
Speaking of improving access, Sidecar is offering health insurance to individuals with greater freedom and flexibility starting in Ohio. These direct-to-individual plans are in the form of ACA plans. Sidecar is adding value by lowering premiums and working with providers to lower the cost of care that is transferred to the individual. A lot of this is done using price transparency and immediate payments upon a visit so that both the individual and the doctor are in sync. This helps eliminate third parties, claims management, and reimbursements and makes it much easier for individuals who generally have a tough time accessing a restricted set of benefits from their employer.
My thoughts
There will be a lot more coming in the payer space. As third parties evolve, solutions similar to Flume will capitalize on specifics in the TPA administration space, bridging the gap between payers and vendors as well as making it much much easier for employers to set up care. More and more people are starting businesses and more of these small businesses/startups will need access to health insurance, and not just access but higher quality care with an average life span increasing and greater awareness of care options that are available today.
On the individual side, there is a lot more room for innovation around point solutions. There are already solutions that are bringing payers closer to employers and individuals for certain care types such as Omada for MSK. With Sidecar, there are also better direct payment options available to the individual without having to sign up for an employer or third party. Point solutions such as mental health, MSK, and fertility care will see the rise of insurance/payment options in addition to care management and access to care itself.



